-
Laparoscopic Hysterectomy in UAE — A Complete Guide by RAK Hospital
-
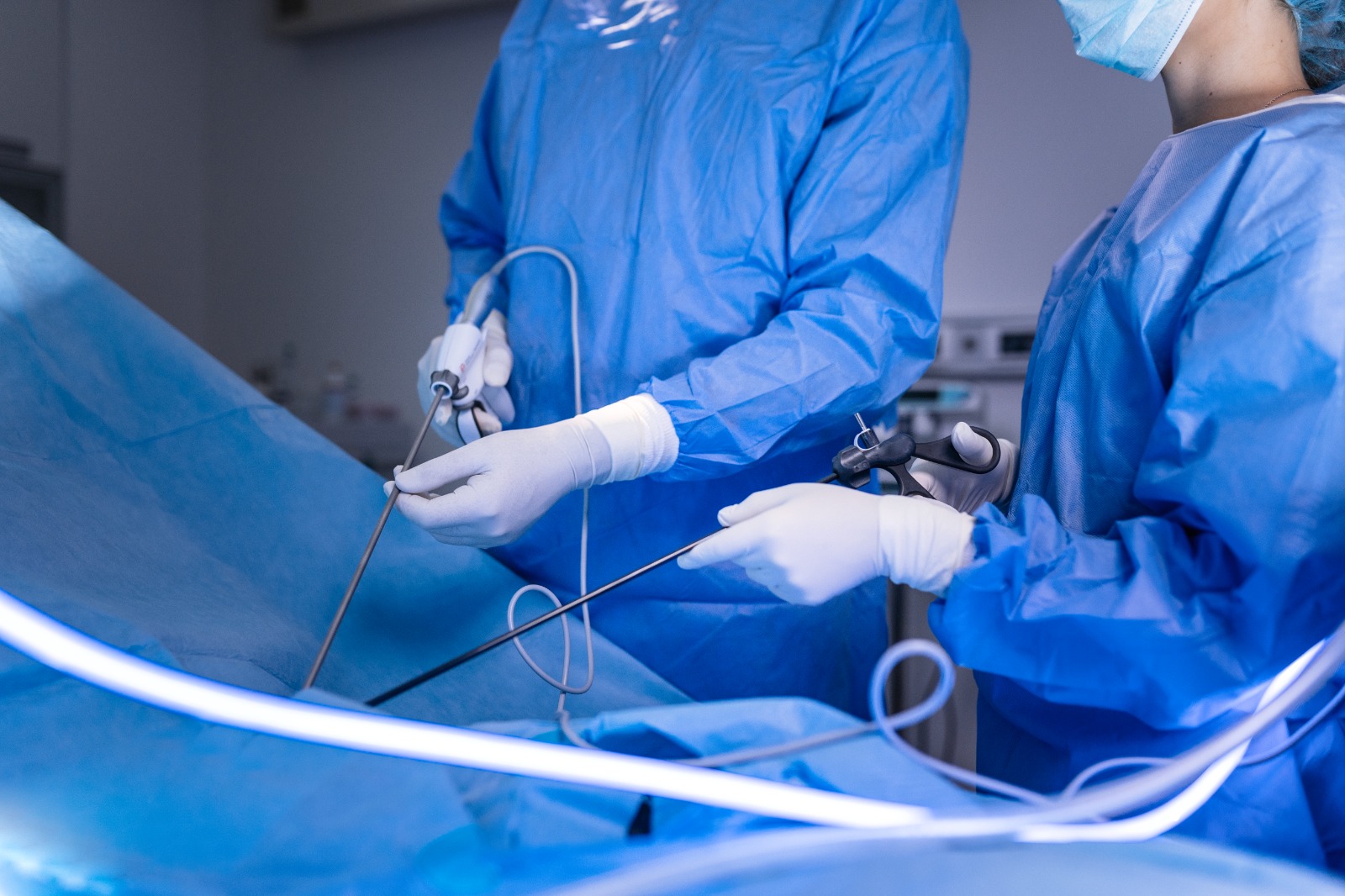

Hi, I’m Dr. Nilesha Chitre, Specialist laparoscopic Gynecologist at RAK Hospital —Here’s What I Want Every Woman to Know About Laparoscopic or minimally invasive or key hole Hysterectomy.
For more than 25 years, I’ve had the privilege of caring for women across India , Maldives, Oman and the UAE, helping them navigate everything from routine gynecologic concerns to complex pelvic conditions. Over the course of my career, I’ve performed hundreds of laparoscopic surgeries, and one thing I see repeatedly is the worry women feel the moment the word “hysterectomy” is mentioned.
Almost every week, I meet patients who arrive with the same anxious questions.
A working woman unable to go to work because of heavy bleeding that leaves her exhausted. A woman in her 40s struggling with fibroids, severe pelvic pain, or pressure. Someone newly diagnosed with precancerous uterine or cervical cancer, terrified at the thought of “surgery to remove the uterus.”
In nearly every consultation, I find myself doing the same thing – helping her understand what a hysterectomy truly is, what it isn’t, and how far surgical techniques have advanced.
That is why I decided to write this blog.
Women deserve clear information, free from fear, myths, and confusion. If you are considering hysterectomy surgery or have been advised to undergo one, you should know exactly what to expect—the procedure, recovery, safety, options available, and how modern laparoscopic techniques have changed outcomes completely.
At RAK Hospital, we use minimally invasive technique for hysterectomy that prioritize quicker healing, precise surgery, smaller incisions, and significantly better comfort. Our team relies on advanced imaging, state of the art laparoscopic systems, and enhanced recovery pathways that have helped thousands of women to enhance their surgical outcome and improve quality of life.
So, let’s begin by understanding the basics.
A laparoscopic hysterectomy is a modern, minimally invasive procedure in which the uterusis removed through a few small incisions in the abdomen. Instead of a large cut, surgeons useathin telescope-like camera (a laparoscope) along with long slender accessory instruments to Internal perform the surgery safely and precisely.
This approach is more advanced and cosmetic compared to traditional methods of hysterectomy:
In the UAE, laparoscopic hysterectomy has quickly become the most preferred option because it helps women heal faster, return to work sooner, and experience far less postoperative discomfort. With the right expertise and technology—as offered at RAK Hospital—most women can go home within 48 hours and recover far more smoothly than with traditional open surgery.
A hysterectomy is never suggested lightly. It is considered when a woman’s symptoms begin to impact her daily life, her health, or her ability to function normally. In many cases, women reach this point after trying medications, hormonal treatment, or physiotherapy without lasting relief.
Large or multiple fibroids can cause heavy bleeding, pelvic pressure, urinary problems, and chronic discomfort. When symptoms become severe or keep returning, removing the uterus becomes a long-term solution.
Endometriosis can lead to ongoing pelvic pain, painful periods, and difficulty with daily activities. When the disease affects deep pelvic structures or keeps recurring despite treatment, hysterectomy may be recommended.
Pelvic pain that continues for months or years – especially when linked to uterine conditions—can significantly impact quality of life. In select cases, removing the uterus offers meaningful relief.
Some women experience prolonged, heavy bleeding that does not improve with medication or minimally invasive treatments. A hysterectomy may stop the bleeding permanently.
When the uterus slips down into the vaginal canal, it can cause pressure, urinary leakage, and difficulty walking or sitting. Surgery to remove the uterus and repair pelvic support may be needed.
In early-stage cervical cancer, removing the uterus – and in some cases surrounding tissues—can be an important part of treatment.
Not every hysterectomy involves removing the ovaries. In fact, in many cases, keeping the ovaries helps maintain natural hormones and prevents early menopausal symptoms. However, removal is recommended when:
Women with strong family history or genetic markers may need preventive removal of the fallopian tubes and ovaries.
If cysts return often or look suspicious on imaging, removing the ovaries may be the safest option.
Occasionally, a severe pelvic infection can damage the ovaries to the point where removal becomes necessary.
Every woman is different. Some women keep their ovaries to preserve hormonal balance, while others may benefit from removing both the fallopian tubes and ovaries to reduce cancer risk or resolve chronic pain.
Your surgeon evaluates:
The goal is always to choose the option that protects your health while ensuring the best possible quality of life.
Different conditions require different surgical approaches. Choosing the right type of hysterectomy is crucial for safety and recovery.
The most common option. Both the uterus and cervix are removed while preserving the ovaries if they are healthy.
The upper part of the uterus is removed but the cervix is left in place. This is sometimes chosen based on patient preference and specific medical needs.
Used mainly for cervical cancer, this surgery removes the uterus, cervix, surrounding tissues, and part of the vagina for complete cancer control.
A combination approach where surgeons use laparoscopy to safely detach the uterus and complete removal through the vagina. Useful for complex cases that still benefit from minimally invasive recovery.
Modern gynecology has shifted strongly toward minimally invasive laparoscopic techniques, especially in the UAE where women prefer quicker healing and minimal downtime.
Here’s why:
1. Small Incisions, Better Comfort
Only tiny cuts are needed, reducing pain and healing time.
2. Less Blood Loss
Precise control minimizes bleeding and improves safety.
3. Lower Risk of Blood Clots
Early mobility and gentler surgery reduce clot risk after the operation.
4. Shorter Hospital Stay
Most women go home within 24 hours—a huge benefit for working women and mothers.
5. Faster Recovery
Many patients resume normal activities within a few weeks after surgery.
6. Less Postoperative Pain
Smaller cuts and minimal internal trauma mean significantly more comfort.
7. Better Cosmetic Outcome
Tiny scars fade quickly and are barely noticeable.
A laparoscopic hysterectomy is a structured, carefully planned procedure. At RAK Hospital, every step is designed to maximize safety, comfort, and precision.
Before the procedure begins, the medical team conducts a complete assessment to understand your symptoms and overall health. This usually includes:
This evaluation ensures that your treatment plan is fully personalised.
The procedure is performed under general anesthesia in a modern, fully equipped laparoscopic suite.
The surgeon creates a few small incisions in the abdomen – usually 0.5–1 cm- which significantly reduces postoperative pain and speeds healing.
A thin camera (laparoscope) is inserted through one of the incisions. This provides a magnified, high-definition view of the pelvic organs, helping the surgeon perform the procedure with exceptional accuracy.
If you are undergoing a total hysterectomy, uterus along with cervix is removed.
The uterus is separated from surrounding tissues using laparoscopic instruments and removed without large incisions. If needed, decisions about removing the fallopian tubes and ovaries are carried out exactly as planned during the evaluation.
Once the procedure is complete, patients are moved to recovery for close monitoring.
The majority of patients can return home within 48 hours post surgery.
Your safety is central to every step of the process.
Healing happens gradually, and it’s important to know what to expect.
Some soreness, abdominal discomfort, and shoulder-tip pain from gas used during laparoscopy are normal. Fatigue is common but improves quickly.
Most women can return to light work and handle everyday household tasks. Energy improves steadily, and walking becomes easier.
Women return to normal routines, including exercise, travel, and work, unless advised otherwise.
Normal:
Call your doctor if you experience:
RAK Hospital significantly minimizes risks through advanced technology, meticulous surgical technique, and experienced minimally invasive surgeons.
| Factor | Laparoscopic Hysterectomy | Abdominal Hysterectomy |
|---|---|---|
| Recovery Time | 2–4 weeks | 6–8 weeks |
| Pain | Much less | Moderate to severe |
| Scars | Tiny small incisions | Large abdominal scar |
| Hospital Stay | Shorter hospital stay (often <48 hrs) | 2–3 days |
| Risks | Lower risk of blood clots, fewer infections | Higher risk |
| When Needed | Most cases | Very large fibroids or extensive cancer |
Laparoscopy or minimally invasive surgery is preferred whenever medically possible.
Many women worry unnecessarily about life after hysterectomy. Here’s the truth:
What Stays the Same:
What Changes:
Hormone-related changes only occur if the ovaries are removed.
I always tell my patients – you’re not alone. A hysterectomy like any organ removal from body is a major decision, and my goal is to help you feel informed, safe, and supported at every step of the way. At RAK Hospital, we combine advanced minimally invasive techniques with compassionate care so you heal comfortably and return to your normal life with confidence.